Understanding Lipedema: Early Diagnosis and Personalized Care
Lipedema is a chronic disorder of fat distribution that primarily affects women, causing disproportionate fat buildup—most commonly in the arms and legs. Over time, this condition can lead to visible deformities, discomfort, and emotional distress. Unfortunately, in its early stages, lipedema often goes unrecognized, leaving many patients to endure years of physical, psychological, and aesthetic suffering before receiving an accurate diagnosis.
Many women with lipedema struggle to be taken seriously, even by medical professionals. But one fact must be clearly understood:
Lipedema is a medical condition that cannot be treated through diet or exercise alone.
To help improve quality of life and reduce suffering, early diagnosis is essential. In some cases, this may require consulting multiple specialists. Once diagnosed, patients can begin appropriate conservative treatments – or, where necessary, pursue permanent removal of the diseased fat through liposuction.
At LipoXpert, our experienced team is here to support you every step of the way – from diagnosis to creating a personalized treatment plan tailored to your unique needs. Whether you’re pursuing conservative care or surgical intervention, we’re committed to providing expert guidance, care, and compassionate support throughout your journey.

The structure of the fatty tissue in the subcutis layer is altered in patients with lipedema. The lymph vessels cannot remove water properly, which can eventually lead to chronic lymphoedema. Moreover, it causes fibrotisation (increase in connective tissue) and scarring of the subcutaneous fatty tissue. These scars are palpable under the skin.
The condition usually starts during puberty, but it can also break out later as a result of hormonal changes. The most common examples are pregnancy, menopause or taking the contraceptive pill. However, these people are usually already predisposed to lipedema.
The most important question first: Is lipedema caused by being overweight? The answer is clearly: No. Lipedema is not caused by a lack of exercise or poor nutrition, but by an uncontrolled change in the fatty tissue. However, concomitant obesity can have a negative impact on the course of the disease.
It has not yet been definitively resolved why lipedema develops in the first place. However, various factors promote the development or severity of lipedema. Concomitant diseases have also been proven.
In many cases, there is a genetic predisposition that is inherited from the family gene pool. This means that, if lipedema occurs in the mother and/or grandmother, there is a high probability that the daughter will also be affected.
The number of fat cells is fixed until the age of 20, after which they only increase or decrease in size. So why does the disease break out after the age of 20? Since it mostly affects women, lipedema is often associated with oestrogen-related changes. Dr Katrin Lossagk, MD answers the most frequently asked questions about the hormonal causes of lipedema:
- To what extent is the development or outbreak of lipedema related to the contraceptive pill?
A connection has not yet been scientifically proven. However, some patients attribute the deterioration or onset of the condition to taking the pill. Such data are not evidence-based. - Is there a link between lipedema and thyroids or hypothyroidism?
Again, there is no evidence-based connection. Nevertheless, for years we have been able to observe an increased incidence of hypothyroidism (insufficient supply of the thyroid hormones triiodothyronine and thyroxine to the body) and Hashimoto’s (inflammation of the thyroid gland) in lipedema patients. - Is there a connection between lipedema and progesterone or progesterone deficiency?
Progesterone deficiency causes a tendency to oedema, and an additional deficiency can make lipedema worse.
The lymph vessels complement the body’s vascular system and transport body fluids, blood cells and nutrients (fats) that are secreted by the cells. In the process, the tiny lymph capillaries absorb tissue water (called lymph) and pass into the larger lymphatic channels and ultimately into the blood vessel system of the superior vena cava.
In lipedema patients, the permeability of the blood vessel capillaries is impaired, which results in more fluid being released into the connective tissue. The fat cells of the subcutis absorb this fluid and put more pressure on the vascular system, creating a vicious cycle and causing even more fluid to be released from the blood vessels. The lymph vessels are compressed and can consequently remove less fluid. This results in an accumulation of water in the tissue, a so-called oedema.
Apart from the aesthetics and the accompanying psychological strain, the physical strain plays a key role. How severe the symptoms of lipedema become varies from person to person. If the disease is not treated, lymphoedema can progress over the years. Regardless of the stage the patient is in, various symptoms can gradually appear.
Often there is a strong feeling of tension and the sensitivity to touch gradually increases – not to mention, the restriction of movement that comes with severely swollen legs. The pressure pain is caused by the accumulation of water in the fat cells, but pain is also caused by inflammation under the skin. Due to the increase in volume, pressure is exerted on the surrounding tissue and tension is created. Consequently, the skin reacts painfully to touch and pressure. The more the lipedema progresses, the more severe the symptoms can become. Legs, arms or hips can then hurt even without applying pressure, and their circumference increases.
Damage to the small blood vessels (microangiopathy), which often occurs in addition to lipedema, can also lead to bruising.
The water that accumulates in the tissue also causes oedema, which makes the tissue very taut. This build-up of water eventually causes pressure pain (tenderness) – a leading symptom of lipedema.
The psychological aspect should not be ignored either. In most cases, people do not realise that the person suffers from lipedema and that the fat deposits are not due to obesity or lack of discipline.
Even some doctors do not take the suffering of their lipedema patients seriously, stirring up further uncertainty and a lack of confidence in potential treatments.
Shame and social isolation as well as depression are frequent consequences or accompanying symptoms of lipedema. In addition, patients’ feelings of a complete loss of control accompanied by massive changes in their daily routine can also have an enormous impact on their psychological wellbeing.
Any pain caused by lipedema is not related to its stage of development. Patients can even suffer from pain in the first stage, when no major changes are visible and the tissue is soft. However, experience shows that this pain increases with the severity of the condition. Stinging and burning are characteristic. In addition to the sensitivity of the skin to pressure, chafing and the resulting inflammation cause pain.
If the arms and legs feel cold or heavy, it is not due to the stage of lipedema; rather it varies from patient to patient.
Some factors temporarily promote the symptoms, making them worse in certain situations:
• Warm weather
• Sauna
• Standing for a long time
• Sitting for a long time
• In the evening
Lipedema is unique in each affected person – both in terms of location and intensity. While some women are only slightly impaired, others may suffer from severe symptoms. Basically, the disease progression can be divided into four stages.
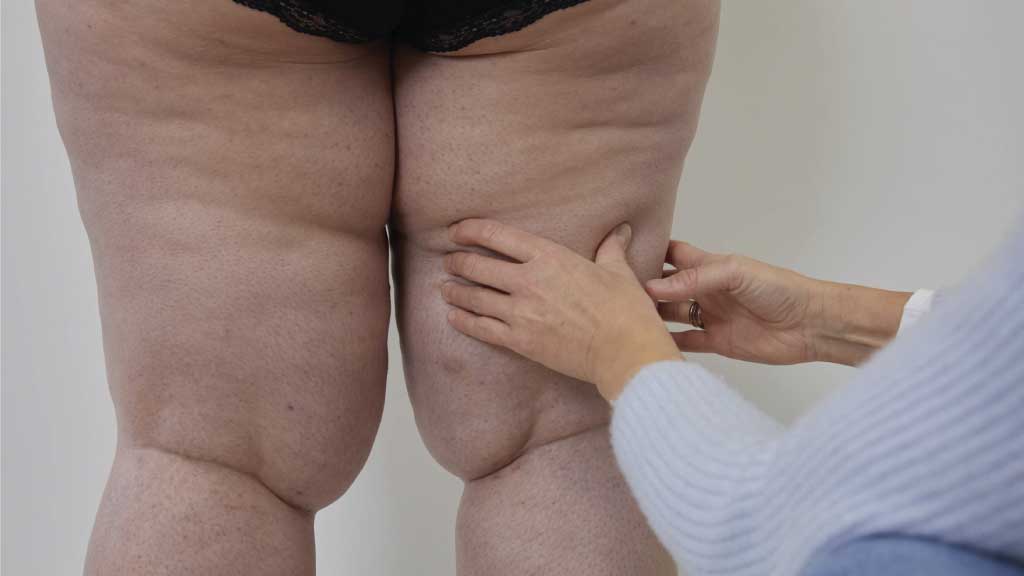
In the first stage of lipedema, the skin is still mostly smooth, but may start to look like an orange peel. Thickened subcutaneous fatty tissue accumulates in the area of the thighs, among other places, which results in so-called saddlebags.
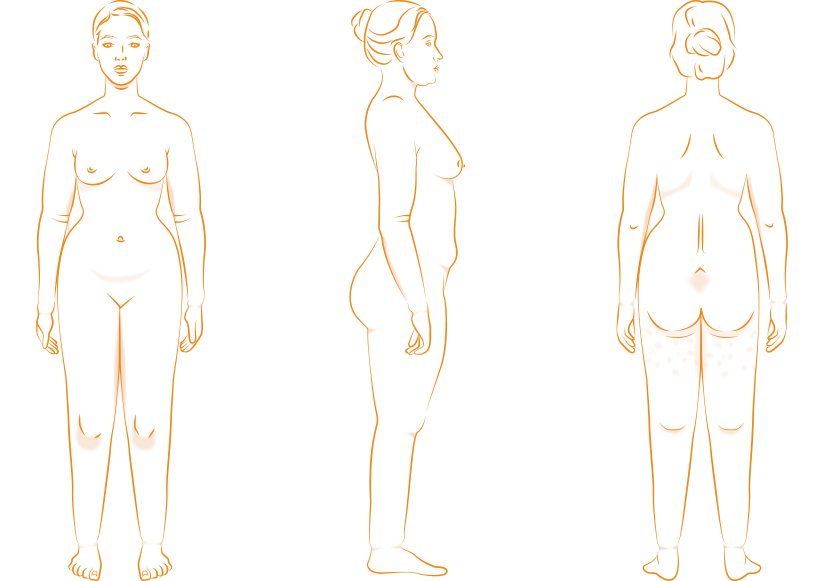
Large fat pads form, fibrosis tissue, which is perceived as ‘painful noodles’ under the skin. The saddlebags become more pronounced and the knees and ankles are clearly thickened.
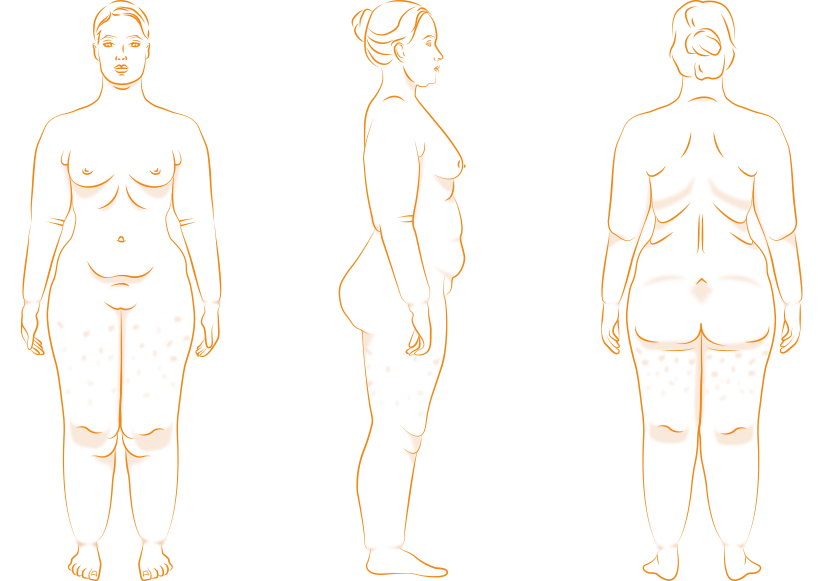
In the third stage of lipedema, the subcutaneous tissue increases uncontrollably and becomes severely hardened. Folds of fat droop on the inner sides of the thighs, knees and ankles, causing chafing and significant restrictions in freedom of movement. The weight of the hanging fat bulges puts additional strain on the joints, which can lead to deformities.
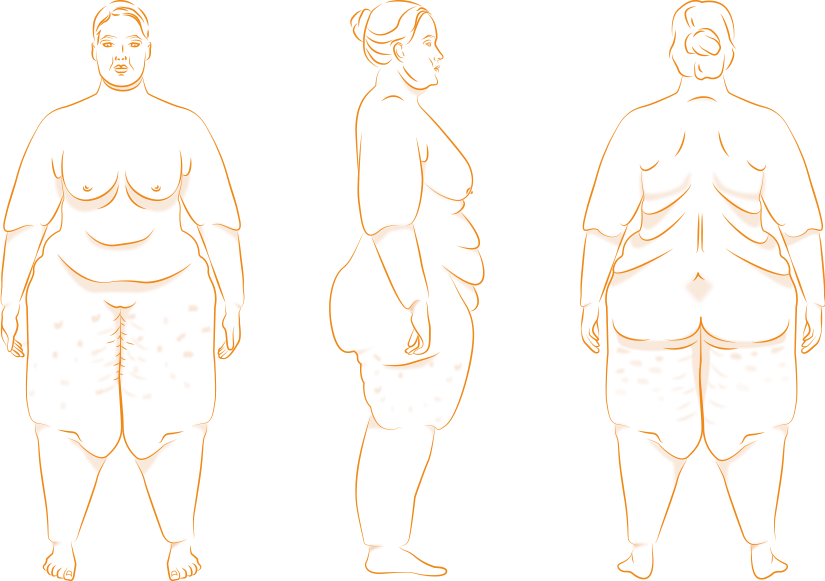
Officially, lipedema is only divided into three stages. However, if lymphoedema also develops, it can be defined as a fourth stage. So-called lipo-lymphoedema, in which fluid builds up in addition to fat, is often the result of lipedema that has gone untreated for a long time.
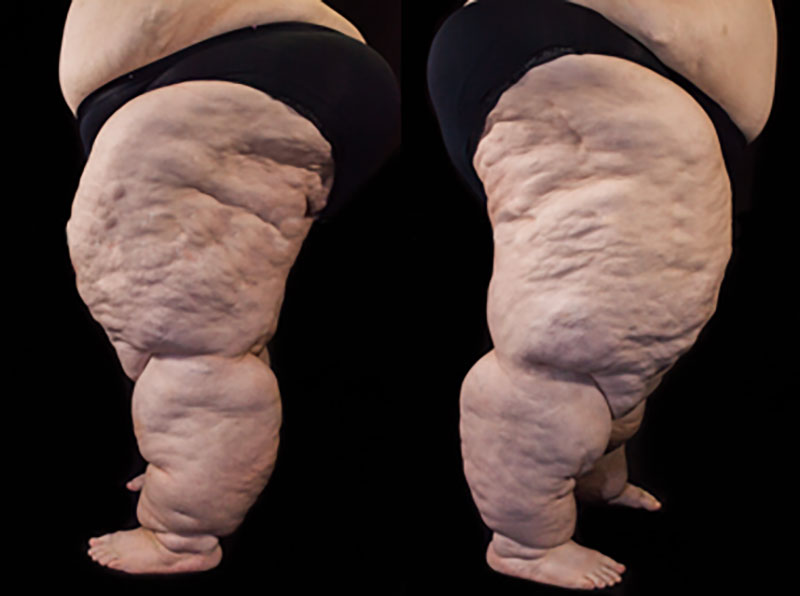
Lipedema can be recognised by an increase in subcutaneous fat tissue, which is usually first distributed on the extremities (legs and arms) and, as the disease progresses, eventually affects the hips and buttocks (in the form of so-called saddlebags) and other areas. The distribution of fat on the legs and arms can vary greatly from person to person. Some patients suffer more from fat increase in the area of the upper or lower legs (or upper or lower arms); in other patients, the entire leg or arm may be affected. However, this fat distribution disorder always occurs symmetrically. Painful fat distribution disorders or increases in volume, even if they have not yet been empirically proven to be lipedema, can affect various parts of the body:
- Legs (thighs, calves, knees)
- Arms
- Buttocks
- Abdomen
- Face (chin, cheek area)
- Breast
- Neck
- Back
We want to help our patients and not get lost in definitions. Therefore, the above mentioned are areas where we have found painful, partly disfiguring and massively impairing fat deposits in patients. We are still talking about diseased areas, but not directly about lipedema areas! Typically, in the course of a surgical lipedema therapy, we observe that a painful accumulation of fat also develops more or less surprisingly in other areas. It is very important to us that we inform our patients about this in good time, i.e. before the first operation.
Lipedema is considered a ‘woman’s disease’. This is partly due to the fact that men have a different adipose tissue structure than women. However, although rare, men can also develop lipedema, for example after hormone therapies, as a result of severe liver disease or due to hormonal disorders. Treatment is the same for any gender.
Not all signs of lipedema appear at the same time or to the same degree. Diagnosis is especially difficult in the first stage. Lipedema is often only recognised when the disease spreads and the symptoms get worse. Unfortunately, the lipedema phenomenon is still largely unknown to many doctors, which explains why it is often confused with obesity.
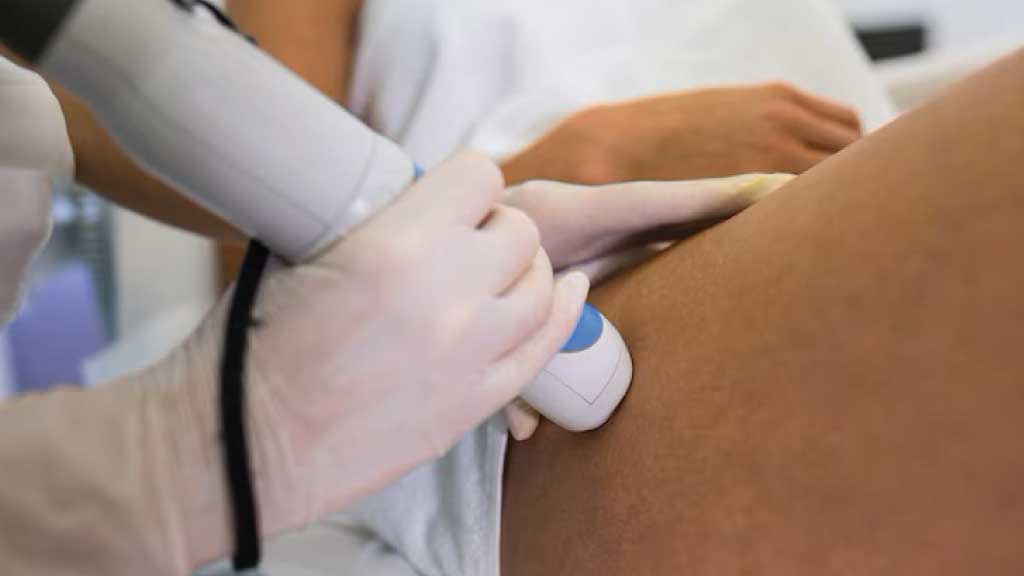
As specialists in lipedema, we have a lot of experience with the pathology and symptoms, allowing us to determine at an early stage whether you are suffering from it. We use a variety of diagnostic methods to do this.
Get an additional professional opinion. If you are unsure or have already consulted other doctors, we offer you the possibility of a second opinion. As experienced lipedema specialists, we are here to answer your questions, provide you with further information and make a detailed diagnosis.
Once Lipedema has been diagnosed, holistic treatment involving various conservative methods is recommended.
These include wearing customized compression garments, which exert targeted pressure on the tissue, support the lymph flow and can slow down the progression of the disease. This is complemented by manual lymphatic drainage, a gentle massage technique that reduces fluid retention and can relieve feelings of tension.
An anti-inflammatory diet, for example with omega-3-rich fish, nuts and fresh vegetables, can promote well-being and reduce inflammation in the tissue. Regular exercise, especially joint-friendly activities such as swimming, cycling or Pilates, also strengthens the muscles and promotes blood circulation. Yoga and meditation can also help to reduce stress and improve general well-being.
So far, lasting relief and even complete freedom from symptoms can only be achieved through liposuction. This targeted surgical procedure completely removes the abnormal fatty tissue, which not only noticeably reduces pain and tenderness, but also allows the appearance of the body silhouette to be adjusted. After the procedure, many lipedema patients report a significant relief in their everyday life and the feeling of finally feeling at home in their own body again.
As mentioned above, people often make false diagnoses or confuse lipedema with obesity. Even with ultrasound measurements, it is difficult to differentiate between the various forms.